 This World Diabetes Day, 14th November 2017, our podiatrists want to highlight the importance of caring for your feet. Good foot care is essential for everyone, more so, if you have diabetes.
This World Diabetes Day, 14th November 2017, our podiatrists want to highlight the importance of caring for your feet. Good foot care is essential for everyone, more so, if you have diabetes.
Those living with diabetes have high glucose levels and amongst other things, these levels can damage blood circulation and can lead to reduced feeling in the feet. Limited feeling in the feet could mean that problems may not be immediately obvious, if left untreated, foot problems can lead to infections and in some cases, more serious issues.
Here we talk about how diabetes can affect the general health of a person diagnosed with the condition, and why regular check-ups, including foot screening are especially important.
What is diabetes?
If you have diabetes, the level of glucose in your blood (sometimes people will talk about the sugar in their blood) is not as well controlled as it needs to be. Normally, your body produces insulin which helps to keep blood glucose levels well controlled, especially after having food or drink or when you haven’t eaten for a while. In diabetes, the insulin produced by your body is not sufficient to control the glucose levels in your blood.
Treatment
In most cases of diabetes starting in later life (Type II), diet control is advised. The aim of this is to choose foods which release glucose in to the blood stream at a slower rate, over a longer period of time, so that the body’s natural insulin can breakdown the glucose more effectively. Weight loss is frequently advised before and after diagnosis of diabetes. Reduction in excess body fat allows insulin to be released and reach the blood stream more effectively.
Medication can be prescribed to help the body produce or use insulin more effectively to breakdown glucose, when diet control is not effective enough.
In a small number of cases, or in younger onset diabetes (usually childhood – known as Type I diabetes), Insulin will be prescribed and administered to boost the body’s failing natural supply.
How does diabetes affect feet?
When blood glucose levels are poorly controlled over a period of time, blood vessels become permanently damaged and blood supply to all parts of your body can be reduced. In the foot, poor blood supply to the nerves can affect the feeling you get in your feet. Numbness, ‘wooliness’ and pins and needles are all common descriptions, but not exclusive. This nerve damage is called peripheral neuropathy.
The arteries, veins and smaller blood vessels including capillaries can be affected, often affecting the feet first of all. If blood supply is reduced to the feet, injuries won’t heal as quickly and the immune system won’t fight infections as well as it should.
If you have diabetes, it is very important that you have a diabetic foot check at least once a year. Your GP will normally arrange for you to have regular checks on your feet, alongside checks for your eyes and blood tests to monitor your kidneys. These are other key areas of the body that may be affected by diabetes. Your GP will arrange blood tests to monitor your blood glucose control – these tests pick up certain markers in your blood which can show how good your control is over a number of months, even though the tests are taken on just one day. Good blood glucose control/diabetes control is the best way to prevent problems arising.
How can I look after my feet if I have diabetes?
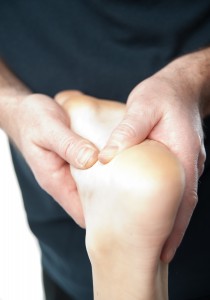 If the sensation in your feet is affected by diabetes, you may not feel injuries when they occur. If left unchecked, they can become increasingly problematic and potentially open wounds may become infected. If your immune system is suppressed the impact of this can be severe. In very extreme cases gangrene can occur.
If the sensation in your feet is affected by diabetes, you may not feel injuries when they occur. If left unchecked, they can become increasingly problematic and potentially open wounds may become infected. If your immune system is suppressed the impact of this can be severe. In very extreme cases gangrene can occur.
It is recommended that you look at your feet daily, using a mirror, if you struggle to get down to see them well. This means that any damage you have not felt, can be treated as soon as possible, to allow a speedy resolution.
If you notice a small wound, graze, blister or similar injury, bathe the area in warm salt water and dress with a clean dry dressing. If the injury starts to get worse, or you notice an increase in redness or swelling, or if it just doesn’t start to improve within a couple of days, we recommend you see a Podiatrist as soon as possible. More often than not, they can do some treatment to allow the wound to start improving, with some localised treatment and application of certain, medical issue dressings which encourage a good healing environment for the affected skin cells. In some instances, it is necessary to see your GP for antibiotics, the podiatrist can advice you if this is required.
Protect your feet from injury by avoiding walking in your bare feet or in plain socks. Before you soak your feet or get in the bath, use your elbow to check the temperature of the water, so you do not scald your feet. Check inside your shoes and boots before you wear them, give them a shake to make sure no stones, pins or tacks have found their way in. Wear socks or stockings to reduce friction and the risk of blisters and sores.
Podiatrists can check the circulation and sensation in your feet and advise you if either of these have reduced. This should be monitored, at least once a year as the situation can change over time. If you notice any of the following, we strongly recommend you see a Podiatrist urgently, or your GP, for advice in the interim.
- Redness and swelling
- Localised temperature increase to one area of the foot
- Red or black discolouration within an area of callous/hard skin
- Fluid or pus exuding from a wound, especially if it has an unpleasant smell
- Non-resolving breaks in the skin
- Ulcerations
If you are a smoker, the combined effect of smoking and poor diabetes control is known to significantly increase your risk of circulation problems to your feet and legs. The severity of these circulation problems will also dramatically increase.
How can Newcastle Sports Injury Clinic help?
At the Clinic one of our Podiatrists can help take good care of your feet. In the initial appointment we will take a comprehensive medical history, including details of the duration of the diagnosis, how it is managed and the current HbA1c levels. This is followed by a thorough assessment of the feet, including vascular, neurological and musculoskeletal examinations. These initial assessments form the baseline from which we can monitor the impact of diabetes on the feet. Depending on our findings, we will arrange to check your feet either annually or every 3 to 6 months. This decision will be based on NICE Guidelines which provides best practice recommendations for all practitioners. This comprehensive approach to diabetic care will mean that we are with you every step of the way.
For further information regarding our support for diabetics please contact 0191 2330500 where one of our Podiatrists will be happy to assist you.
References: www.socap.org, www.givingupsmoking.co.uk

